You Can’t Handle the [BMI] Truth
As of 2010, approximately 70% of Americans were either overweight or obese as defined by their Body Mass Index or BMI. Obesity related health issues are significant because they increase health care costs, decrease productivity and result in premature death. Discussing BMI invokes a great deal of passion because it creates undesirable classifications for some (overweight and obese).
As accurate as the BMI label is for many, no one wants to be designated as unhealthy, overweight or obese, especially when their own lifestyle choices have lead to those classifications. Rather than accept the truth and change, many simply point to flaws in BMI (even flaws that are completely irrelevant for their own circumstances) making it much easier to justify unhealthy actions and dismiss the negative BMI classification. It’s much easier to criticize than change unhealthy habits.

For some, an even more appealing avenue than denial is constructing a reality in which the scientific evidence proving how unhealthy a fat, overweight and obese lifestyle is, is ignored or refuted. BMI isn’t the end of the road. If BMI classifies you as overweight, obese and unhealthy, there are other assessments you can take to ensure BMI is giving you an accurate picture.
Too often, many hear bad BMI news, criticize the assessment and turn to the pseudo-science nonsense, health at every size (HAES) which claims size isn’t a good measure of disease risk. When BMI is high, chances are other markers of health are also poor: blood pressure, fasting glucose, body fat, waist circumference and fitness levels. When all the evidence points in a certain direction, you should listen and take action rather than deny and continue on a self destructive path.
BMI 101
Body Mass Index (BMI) is a quick and simple way to gauge disease risk. BMI is a number calculated from an individual’s weight and height corresponding to a certain range: underweight, normal, overweight and obese. Individuals with higher BMIs are at an increased risk for obesity related issues such as: heart disease, hypertension, type 2 diabetes, stroke, sleep apnea, respiratory issues and some forms of cancer.
BMI is a relationship between weight and height:
- BMI Formula = weight (pounds) / (height (inches))2 x 703
The resulting BMI puts an individual in a certain classification:
- Below 18.5: Underweight
- 18.5-24.9: Normal
- 25-29.9: Overweight
- 30+: Obese
BMI predicts disease risk; it’s not a diagnostic tool. BMI predicts disease risk because it’s an indirect measure of body fat percentage. People who have a high body fat percentage are at an increased risk of developing obesity related health issues. You might be wondering: if BMI indirectly measures body fat percentage, why not cut out the middle man (BMI) and deal directly with the real health issue: excessive body fat.
Why is BMI used instead of body fat?
Whenever you hear or read a news report on the official (and alarming) obesity statistics from the Centers for Disease Control and Prevention (CDC), BMI is at the center of the story. BMI is a quick and cheap way to gauge health risk for individuals and populations. It’s a frequently used tool because it’s easy, quick and cheap to measure. It requires no special equipment beyond a scale and measuring tape (for height).
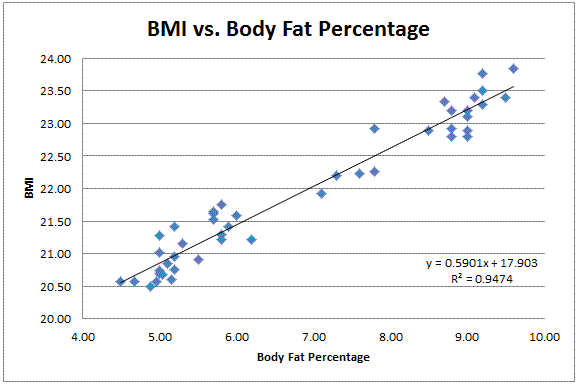
BMI vs. Body Fat Percentage
If body fat is the real issue, why are we using BMI so frequently? BMI is very easy to measure. All you need is a scale to measure body weight and a calculator to plug the numbers into. Body fat is much more difficult to assess and the numbers aren’t always accurate.
Body fat is impossible to directly measure (on someone who’s alive). We use skinfolds, bioelectrical impedance, X-rays and underwater weighing to indirectly measure body fat. Because these measurements are indirect, there’s a certain amount of error associated with each.
A DXA (bod pod) scan uses X-rays to measure bone density and body fat. Unfortunately, it requires expensive equipment and isn’t as simple as measuring body weight (for a BMI calculation). Skinfold accuracy is highly dependant on the person performing the assessment. Bioelectrical impedance results vary with water weight. Body fat is much more difficult, costly and time consuming to accurately measure than BMI.
From my own experience, BMI and body fat percentage have correlated very nicely with eachother. An R2 value of 0.9474 means there’s a very good correlation between the two variables.
Why is BMI so hated?
BMI is hated because it’s the bearer of bad news. BMI labels you as normal or unhealthy; no one wants to be part of the unhealthy group. Ignorance is bliss and many people would rather fight BMI than face and change their own unhealthy lifestyle choices.
When is BMI inaccurate?
BMI is calculated from body weight. Body weight is made up of both fat and muscle. Because BMI is “blind,” it cannot differentiate between the two. As far as health is concerned, the enemy is body fat, not muscle. Certain populations such as athletes or bodybuilders have much more muscle mass than the average person. This extra muscle mass increases body weight but does not necessarily increase body fat.
Since BMI is only calculated from weight, a muscular person can have a high BMI. But does a muscular athlete with a high BMI mean they’re unhealthy? The CDC says athletes are unlikely to have high body fat if their BMI falls in the overweight category (25-29.9). If however, their BMI falls in the obese category (30+), it is likely they are carrying excessive body fat, increasing their risk of obesity related health issues.
Athletes or other muscular individuals who are in the overweight category most likely have nothing to worry about. Those in the obese category are more likely to have a high body fat percentage, putting them at a higher risk of obesity related health issues.
BMI doesn’t always give an accurate assessment for muscular populations (athletes and bodybuilders). All too often, those with an extremely high body fat percentage use this flaw to invalidate BMI for their own situation.
Their logic goes something like this, “If BMI is inaccurate for athletes who workout six times per week and eat healthy, it must also be inaccurate for me, even though I don’t workout and eat some very bad foods.” If you’re confused about whether BMI is giving you a fair picture of health risk, there are other relatively simple health assessments you can take to ensure your lifestyle is putting you on the right track.
Ensure BMI is Accurate For You
BMI is one of the easiest health assessments to perform which is why it’s used so frequently. If you’re doubtful about your BMI classification, there are other ways of measuring health risk. However, when BMI is high, chances are these other health markers will also paint an unhealthy picture.
Body Fat. Excessive body fat is health’s enemy. Measuring body fat provides more insight into health than the blind BMI assessment. There are a few ways to measure body fat, though most are either expensive and require sophisticated equipment or inaccurate.
- Skinfold – A personal trainer typically performs skinfold assessments though anyone who is trained can help you. This assessment involves measuring skinfolds with a caliper on certain areas of the body and using those measurements to calculate body fat percentage. This method is inexpensive and quick to perform but somewhat inaccurate and very inconsistent. Measurements vary based on how well the person performing the assessment takes the measurements. If possible, get the same person to perform this assessment on you over a long period of time for improved consistency.
- Bioelectrical Impedance – This method of body fat testing is more accurate and consistent than the skinfold. Bioelectrical impedance body fat devices are found in body weight scales or hand held monitors. They are relatively inexpensive. Measurements can vary with changes in water weight. It’s important to measure yourself at the same time each day to improve consistency.
- Bod Pod – The bod pod uses X-rays to measure bone density and body fat percentage. This method is fairly accurate but requires sophisticated equipment and is therefore expensive. These machines are typically found in gyms and medical centers.
All body fat assessments have some degree of error. When measuring body fat, take note of the trend over a long period of time rather than one measurement.
The American Council on Exercise published general body fat categories. Most people should reside within the athletic and fitness categories:
Classification Women (% body fat) Men (% body fat) Essential Fat 10-13% 2-5% Athletes 14-20% 6-13% Fitness 21-24% 14-17% Average 25-31% 18-24% Obese 32% and higher 25% and higher
Waist Circumference. Waist circumference is a quick assessment which the National Institutes of Health (NIH) notes can help screen for possible health risks that come with obesity. If body fat is stored around the waist rather than the hips, you’re at an increased risk for obesity related health issues.
A high BMI alone increases health risk. A high BMI coupled with a large waist circumference greatly increases health risk. A large waist circumference is defined as 40 inches or higher for men and 35 inches or higher for women. Instructions to measure waist circumference from the NIH: “To correctly measure your waist, stand and place a tape measure around your middle, just above your hipbones. Measure your waist just after you breathe out.”
Fitness Tests. Fitness levels are great predictors of overall health. Those who are slightly overweight but perform well at cardiovascular exercises are generally healthy. In other words, a high level of fitness negates some extra body weight. Fitness is a better indicator of health than weight alone. A few fitness assessments you can perform include the 12 minute run, 1 mile walk, 1.5 mile run, or any of the military PT tests. ExRx has an entire page devoted to fitness testing.
Medical Exam. A medical exam is also a great way to gauge overall health. A healthcare provider can measure blood pressure and order a blood test for fasting glucose and cholesterol levels.
The Bottom Line
BMI is a good, but not perfect, assessment of overall health. Though there is a small population (muscular athletes and bodybuilders) for which BMI is somewhat inaccurate, this flaw is irrelevant for the vast majority of people who are classified as overweight and obese.
BMI is a quick and easy starting point at defining health risk. When health is in question, assessments such as body fat measurements, waist circumference, fitness tests and medical exams can substantiate or refute a BMI classification. Change starts with acknowledging there is a problem. BMI isn’t meant to humiliate or berate you, it’s meant to educate and motivate. Rather than dismiss BMI as inaccurate, use it as a starting point to look into your health. Knowledge is a powerful catalyst for change.